Leading through advocacy, education, and relationships
Diabetes Distress Moderates the Relationship between Quality of Life and Self-Care in Adults with Type 1 Diabetes
Category: 2020
Author: DeWitt Jones
Institution Affiliation: Ohio University Heritage College of Osteopathic Medicine
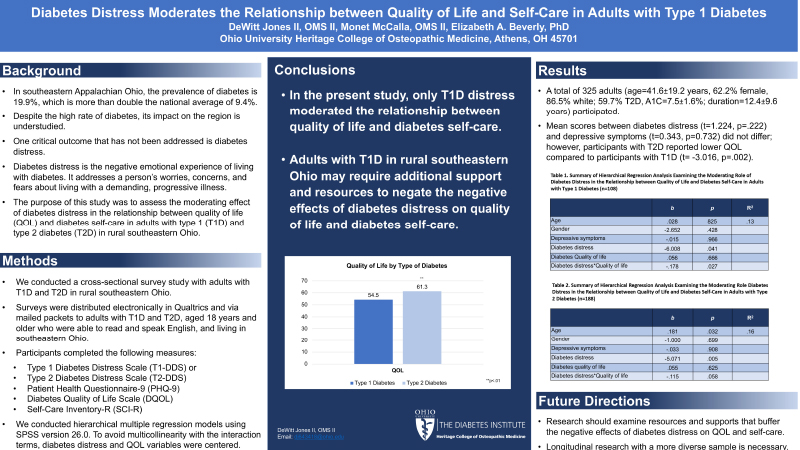
Introduction: In southeastern Appalachian Ohio, the prevalence of diabetes is 19.9%, more than double the national average of 9.4%. Despite the high rate of diabetes, its impact on the region is understudied. One critical outcome that has not been addressed is diabetes distress. Diabetes distress is the negative emotional experience of living with diabetes. It addresses a person’s worries, concerns, and fears about living with a demanding, progressive chronic illness. Objective: The purpose of this study was to assess the moderating effect of diabetes distress in the relationship between quality of life (QOL) and diabetes self-care in adults with type 1 (T1D) and type 2 (T2D) diabetes. Methods: Participants completed the Diabetes Distress Scale for T2D or T1D, the Patient Health Questionnaire-9, the Diabetes Quality of Life Scale, and the Self-Care Inventory-Revised. We conducted hierarchical multiple regression models using SPSS version 26.0. To avoid multicollinearity with the interaction terms, diabetes distress and quality of life variables were centered. Results: A total of 325 adults (age=41.6±19.2 years, 62.2% female, 86.5% white; 59.7% T2D, A1C=7.5±1.6%; duration=12.4±9.6 years) participated. Mean scores between diabetes distress (t=1.224, p=.222) did not differ; however, participants with T2D reported lower QOL compared to participants with T1D (t= -3.016, p=.002). In the T1D model, the interaction between diabetes distress and QOL (b= -.178, p=.027, R2Δ=0.04) was statistically significant, indicating that diabetes distress moderated the relationship between QOL and diabetes self-care. In the T2D model, the interaction between diabetes distress and QOL was not significant (b= -.115, p=.058, R2Δ=0.02), suggesting no moderating effect. Conclusion: In the present study, only T1D distress moderated the relationship between quality of life and diabetes self-care. Adults with T1D in rural southeastern Ohio may require additional support and resources to negate the negative effects of diabetes distress on QOL and diabetes self-care.
Watch Video
 Phone: 567-712-0697
Phone: 567-712-0697
